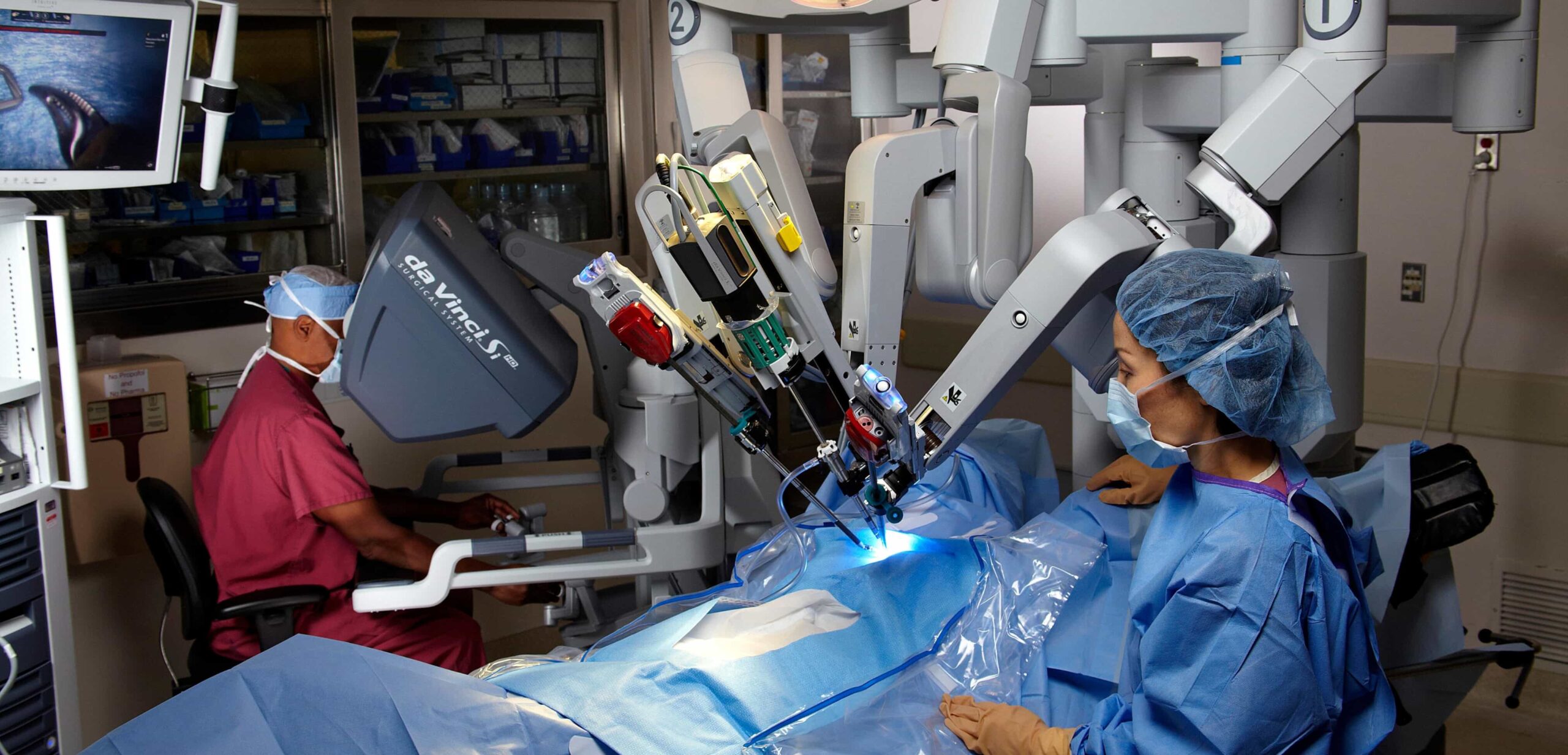
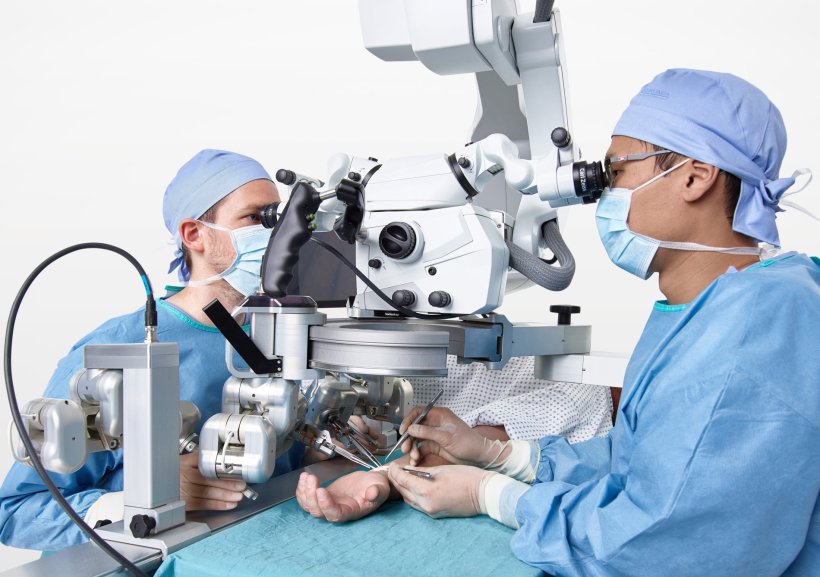
United States, February 9, 2026 — Parliament News — As artificial intelligence enters the operating room, reports of botched surgeries and misidentified body parts are prompting urgent debate across the United States. In 2026, AI surgery risks have emerged as a critical issue for hospitals, regulators, and patient advocates as AI assisted systems become more deeply embedded in surgical care nationwide.
Medical centers across the country are rapidly adopting advanced software and robotic platforms designed to enhance precision and efficiency. Yet recent incidents have raised concerns about whether safeguards are sufficient when algorithms are allowed to influence life critical decisions.
Artificial Intelligence Becomes a Surgical Partner
Artificial intelligence has steadily expanded its role in American healthcare over the past decade. Initially confined to diagnostics and administrative support, AI has now crossed into the operating room, where it assists with imaging analysis, surgical planning, and real time monitoring.
Surgeons use AI tools to map anatomy, anticipate complications, and guide robotic instruments with unprecedented accuracy. However, specialists warn that AI surgery risks increase when clinicians rely too heavily on automated guidance without fully understanding system limitations.
The operating room is an unpredictable environment, and technology trained on historical data may struggle when faced with unexpected variations.
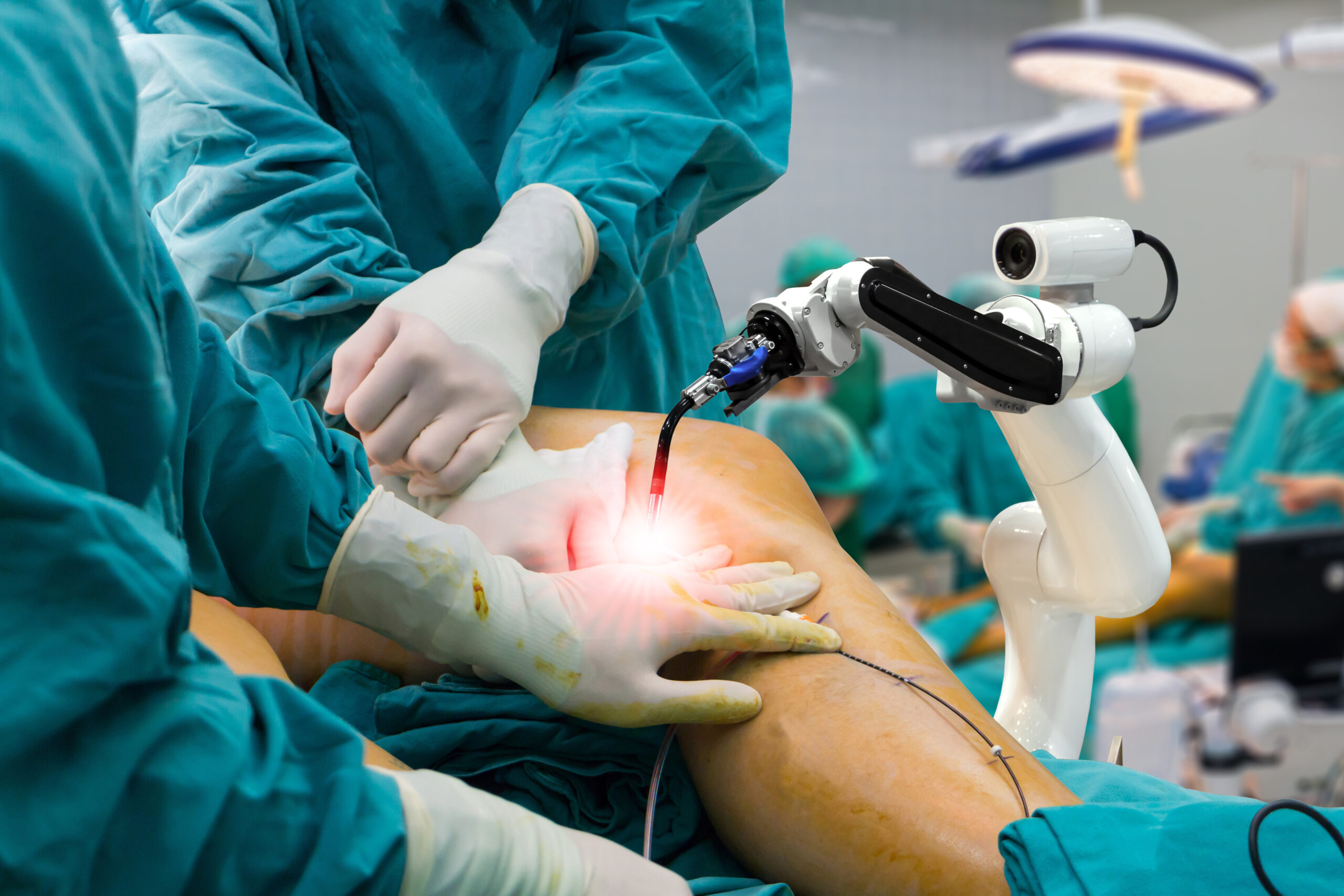
Surgical Errors Draw National Attention
In several states, hospitals have acknowledged internal safety reviews following unusual surgical outcomes involving AI supported systems. While details vary, common themes include delayed recognition of anomalies and over confidence in automated recommendations.
Patient safety experts say these cases illustrate how AI surgery risks can surface when human oversight is reduced. Although many procedures were corrected before causing severe harm, the incidents have intensified scrutiny at the federal level.
Healthcare leaders emphasize that transparency is essential to maintaining public trust as technology adoption accelerates.
Misidentified Anatomy and Data Dependence
One of the most troubling issues involves the misidentification of anatomical structures during AI guided procedures. Artificial intelligence systems depend heavily on data quality, and errors in labeling or imaging can lead to incorrect conclusions.
Clinicians note that AI surgery risks rise when algorithms encounter patients whose anatomy does not match training datasets. This is especially relevant in emergency surgeries, where time pressure limits opportunities for manual verification.
Calls are growing for more rigorous testing across diverse patient populations.
Federal Oversight and Regulatory Gaps
US health regulators are under increasing pressure to adapt existing frameworks to address AI driven medical tools. Current approval processes focus on pre market testing, but critics argue that real world performance demands closer attention.
Lawmakers and medical boards are examining how AI surgery risks should be monitored after deployment, including whether hospitals should be required to report AI related incidents separately from traditional surgical complications.
Washington has become a focal point for policy discussions aimed at strengthening patient protections without stifling innovation.
Accountability in High Tech Medicine
As artificial intelligence assumes a greater role in surgical care, questions of accountability have become more complex. Surgeons remain responsible for procedures, but hospitals select systems and developers design algorithms.
Legal experts argue that unclear responsibility can amplify AI surgery risks, as fragmented accountability may delay corrective action. Some patient advocates are pushing for clearer liability standards that reflect shared responsibility across the technology chain.
The debate underscores the need for legal clarity as medicine enters a new technological era.
Voices From the Front Lines
Medical professionals and safety advocates are increasingly vocal about the need for balance.
“Artificial intelligence should support surgeons, not replace their judgment,”
said a senior US surgical safety specialist.
Another hospital leader noted,
“Technology can enhance care, but it must never outrun safety.”
A patient rights advocate warned, “If AI surgery risks are ignored, public confidence in medical innovation will erode.”
Impact on Patient Trust
Public perception plays a critical role in the adoption of new medical technologies. Surveys indicate that while many Americans are optimistic about innovation, they also expect strict safeguards when technology is involved in surgery.
Awareness of AI surgery risks has led some patients to request additional information before consenting to procedures. Hospitals are responding by updating consent forms and increasing communication around how AI systems are used.
Trust, experts say, must be earned through openness rather than marketing claims.
Hospital Safety Measures and Training
In response to growing concern, several major hospital networks have introduced new safety protocols. These include mandatory human confirmation steps, enhanced monitoring during AI assisted procedures, and expanded training programs for surgical teams.
Reducing AI surgery risks requires clinicians who understand when to rely on technology and when to override it. Medical schools and residency programs are now incorporating AI literacy into their curricula.
Education is increasingly seen as a cornerstone of safe implementation.
A History of Technology Transforming Surgery
Throughout medical history, new technologies have reshaped surgical practice. From the introduction of anesthesia to the rise of minimally invasive techniques, innovation has often been accompanied by periods of adjustment and risk.
The current debate echoes earlier transitions, when unfamiliar tools introduced unforeseen complications. AI surgery risks reflect a familiar pattern in which progress demands recalibration before standards stabilize.
History suggests that careful oversight and gradual integration are essential to sustainable change.
The Road Ahead for AI in US Hospitals
Despite challenges, most experts agree that artificial intelligence will remain a central part of future healthcare. The question is how to integrate it responsibly within existing clinical frameworks.
Managing AI surgery risks will depend on robust regulation, continuous monitoring, and strong collaboration between technologists and clinicians. Policymakers are expected to play a decisive role in shaping standards over the coming years.
The United States now stands at a crossroads in medical innovation.
A Defining Test for Modern Healthcare
The debate unfolding in 2026 represents more than a technical challenge. It is a test of how society balances innovation with responsibility in settings where human lives are at stake.
Handled wisely, artificial intelligence could enhance surgical care. Mishandled, AI surgery risks could undermine trust and outcomes alike.
The decisions made today may shape the future of American healthcare for generations.